Always choose a Position that YOU ARE MOST COMFORTABLE with.
 The Cradle Hold
The Cradle Hold
This classic breastfeeding position requires you to cradle your baby’s head with the crook of your arm. Sit in a chair that has supportive armrests or on a bed with lots of pillows. Rest your feet on a stool, coffee table, or other raised surface to avoid leaning down toward your baby. Hold her in your lap (or on a pillow on your lap) so that she’s lying on her side with her face, stomach, and knees directly facing you. Tuck her lower arm under your own.
If she’s nursing on the right breast, rest her head in the crook of your right arm. Extend your forearm and hand down her back to support her neck, spine, and bottom. Secure her knees against your body, across or just below your left breast. She should lie horizontally, or at a slight angle.
Best for: The cradle hold often works well for full-term babies who were delivered vaginally. Some mothers say this hold makes it hard to guide their newborn’s mouth to the nipple, so you may prefer to use this position once your baby has stronger neck muscles at about 1 month old. Women who have had a cesarean section may find it puts too much pressure on their abdomen
=======================================================
 The Cross-Cradle or Football Hold
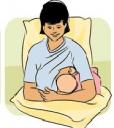
The Cross-Cradle or Football Hold
In this position you tuck your baby under your arm (on the same side that you’re nursing from) like a football or handbag. First, position your baby at your side, under your arm. She should be facing you with her nose level with your nipple and her feet pointing toward your back. Rest your arm on a pillow in your lap or right beside you, and support your baby’s shoulders, neck, and head with your hand. Using a C-hold (see picture), guide her to your nipple, chin first. But be careful — don’t push her toward your breast so much that she resists and arches her head against your hand. Use your forearm to support her upper back.
Best for: You may want to try this hold if you’ve had a Cesarean section (to avoid having the baby rest on your stomach). And if your baby is small or has trouble latching on, the hold allows you to guide her head to your nipple. It also works well for women who have large breasts or flat nipples, and for mothers of twins.
=======================================================
For those of you who prefer to see the positions demonstrated, you can see this video. There are alot of pointers mentioned in the video. So mummy, tune up the volume and make sure you are paying attention.
=======================================================
 Side Lying Down Position
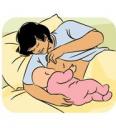
Side Lying Down Position
To nurse while lying on your side in bed, ask your partner or helper to place several pillows behind your back for support. You can put a pillow under your head and shoulders, and one between your bent knees, too. The goal is to keep your back and hips in a straight line. With your baby facing you, draw her close and cradle her head with the hand of your bottom arm. Or, cradle her head with your top arm, tucking your bottom arm under your head, out of the way. If your baby needs to be higher and closer to your breast, place a small pillow or folded receiving blanket under her head. She shouldn’t strain to reach your nipple, and you shouldn’t bend down toward her.
Best for: You may want to nurse lying down if you’re recovering from a cesarean or difficult delivery, sitting up is uncomfortable, or you’re nursing in bed at night or during the day
For me? The Cradle because I was most comfortable in it. For Matin’s mummy, its definitely the Side Lying Down Position and she often continues her sleep while little Matin is nursing, she still does that for her second son, Hadi.
What is your favourite position?
Copyright © 2007-2026 All About Your Child. The contents on this blog are the sole property of the author, Angeline Foong, and may not be used or reproduced in any manner without consent. All Rights Reserved.



